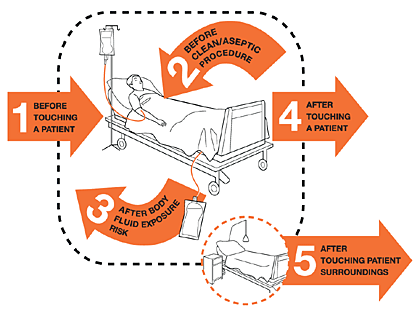
Hospital-acquired infections (HAIs) are a major safety concern for both health care providers and patients.
The US Center for Disease Control and Prevention identifies that nearly 1.7 million hospitalized patients annually acquire healthcare-associated infections (HCAIs) while being treated for other health issues and that more than 98,000 patients (one in 17) die due to these. Several studies suggest that simple infection-control procedures such as cleaning hands with an alcohol-based hand rub can help prevent HCAIs and save lives, reduce morbidity, and minimize health care costs. - NCBI
Ultimately, it is up to the health care personnel involved in patient care and those responsible for surveillance to ensure that adequate measures are being taken to control and ideally prevent infections in the hospital.
The fundamental components of infection control in all healthcare facilities are:
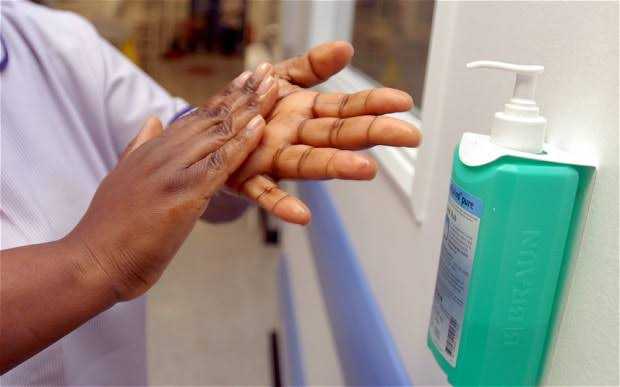
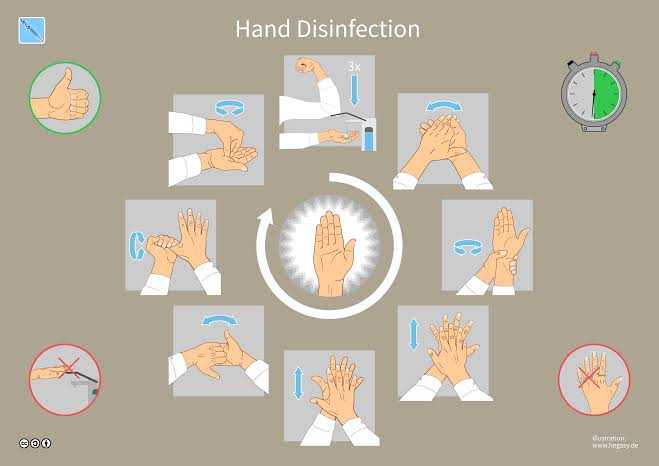
- Hand hygiene
- Sterilization
- Cleaning
- Disinfection
- Personal Protective Equipment (PPE)
All of the above are addressed in the checklist and applied to all areas of the facility including patient rooms, break rooms, and general areas throughout the building.
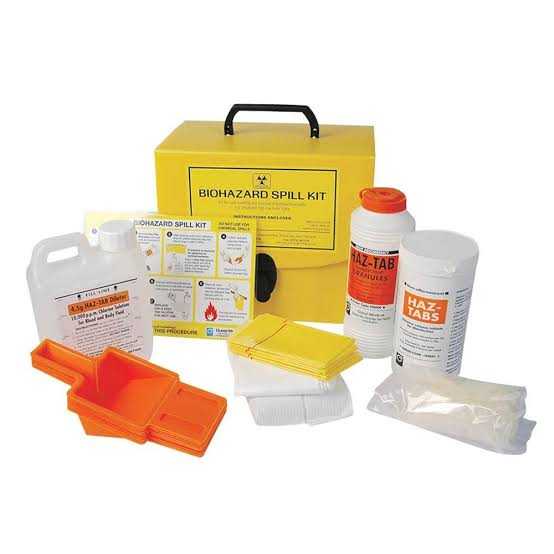
If infectious waste is inadequately managed, harmful microorganisms can be transmitted by direct contact, in the air, or by a variety of vectors, putting the health of hospital personnel, and patients, at risk.
By running this checklist, you ensure that everything is being done to control and minimize the spread of infectious waste throughout your healthcare facility.
Let's get started.
In case you're wondering what Process Street is all about...
Process Street is superpowered checklists. By using our software to document your processes, you are instantly creating an actionable workflow in which tasks can be assigned to team members, automated, and monitored in real-time to ensure they are being executed as intended, each and every time.
The point is to minimize human error, increase accountability, and provide employees with all of the tools and information necessary to complete their tasks as effectively as possible.